FAQ: What health insurance covers
All plans offered to people who purchase their own health insurance must include a core set of Essential Health Benefits, as shown in the chart below.
| Essential health benefit | Example |
|---|---|
| Preventive, wellness, and disease management services | Yearly physical, flu shot, gynecological exam, birth control |
| Emergency care | Treatment for broken bones, heart attacks, and more at a hospital emergency room |
| Ambulatory services | Minor surgeries, blood tests, X-rays |
| Hospitalization | Treatment at a hospital for a condition that requires you to stay overnight or multiple days |
| Maternity and newborn services | Care through the course of a pregnancy, delivery of the baby, and checkups after the baby is born |
| Pediatric services, including dental and vision | Well visits, shots to prevent serious health conditions, teeth cleanings and exams, frames, lenses |
| Prescription drugs | High blood pressure medicine, insulin, antibiotics, birth control pills |
| Laboratory services | Blood tests |
| Mental health and substance abuse services, including behavioral health treatment | Getting help to deal with conditions like depression, alcohol abuse, and drug abuse |
| Rehabilitation and habilitation services | Physical therapy, speech therapy, occupational therapy |
In addition, insurers will cover 100 percent of the cost of many preventive services, such as wellness visits, immunizations, screenings for cancer, and other diseases if the services are received from an in-network provider. That means you will not pay any deductible, copayments, or coinsurance for many preventive services that can help you stay healthy. To learn more how deductibles, copayments, or coinsurance could play a role in your medical care, compare our health insurance plans.
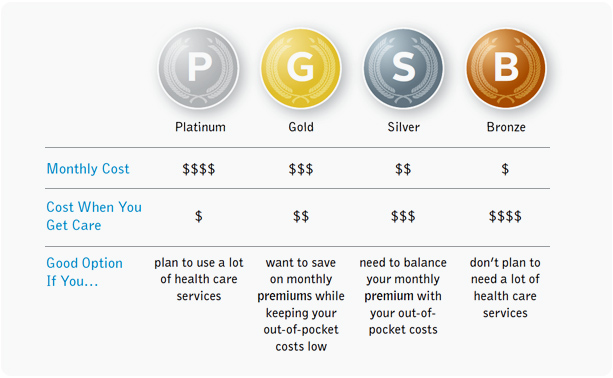
With the Affordable Care Act, the federal government created four categories of coverage — metallic levels — for health plans offered to small businesses (2 – 50 employees) and for people who purchase their own insurance. Plans are assigned one of these metallic levels based on what percentage of the cost of health care services is covered by the health insurance company. These categories — bronze, silver, gold, and platinum — make it easier for you to compare health plans across health insurance companies. All products cover Essential Health Benefits like doctor visits, prescription drugs, X-rays, and hospital stays. The major differences are in what you pay when you need these services and the monthly cost of the health plan. Learn how to shop for health insurance plans.
How the metallic levels compare on costs:
Pediatric vision benefits cover in-network care only for children up to age 19. In-network benefits are covered when you visit a Davis Vision provider. Independence Blue Cross Vision Care is administered by Davis Vision, an independent company.
A separate card is not provided for pediatric vision coverage.
Pediatric vision coverage will be terminated the last day of the month in which he or she turns 19. You can purchase an Adult Vision plan for a dependent who turns 19 and is no longer eligible for pediatric vision coverage.
Routine dental care for adults is not covered in our individual health plans. Routine dental care for children under age 19 is considered an essential health benefit and is available with all plans. To learn more, refer to the Benefits at a Glance for each plan. You can also explore the Adult Dental plans that can be purchased in addition to medical coverage. These plans offer the benefits you need to support prevention, early diagnosis, and treatment for good oral health.
Pediatric dental benefits are in-network coverage only for children up to age 19. Independence Blue Cross dental plans are underwritten by QCC Insurance Company.
A separate card is not provided for pediatric dental coverage.
Pediatric dental coverage will be terminated the last day of the year in which he or she turns 19. Adult dental plans can be purchased for these dependents.
Yes. You are covered for medically necessary services for unexpected illnesses or emergency care no matter where you are. Learn more about your emergency care options.
Mental health and substance abuse services, including behavioral health treatment, are considered an essential health benefit and available with all plans.
Our condition management program supports members who have chronic conditions at no additional cost. Condition management includes:
- Information and support when you are facing medical decisions or treatment options
- Help when you are living with chronic conditions such as diabetes or asthma
- Personal 24/7 support from Independence Blue Cross Registered Nurse Health Coaches, who can look at your condition(s), prescription drugs, recent diagnostic or therapeutic activities, and patterns of treatment and offer meaningful assistance as they support you through the health care spectrum. Health Coaches can provide:
- Information on everyday health concerns, such as headaches and joint pain
- Personalized calls about chronic conditions or health concerns
- Information about what types of questions to ask the doctor
All health plans include a Preventive Plus benefit with $0 member cost-sharing (no copayment, deductible, or coinsurance) when a member receives a preventive colonoscopy1 to screen for colorectal cancer at a Preventive Plus provider. Preventive Plus providers are not hospital-based, and the preventive colonoscopy is performed by a Preventive Plus professional (a gastroenterologist or a colon and rectal surgeon). To find an in-network Preventive Plus providers, use our Find a Doctor tool.
The Preventive Plus benefit does not apply if you reside or travel outside our service area and access care through the BlueCard® Program or the Away From Home Care® Guest Membership Program. If this applies to you, a preventive colonoscopy to screen for colorectal cancer will be covered at no cost when you use an in-network provider. If you choose to use an out-of-network provider, cost-sharing for your plan’s out-of-network benefit applies, and your out-of-pocket costs may be significantly higher.
With virtual care from Teladoc Health (Teladoc), you have a quick, convenient, and affordable care option — you’ll pay $0 for a virtual visit.3 You can reach a board-certified doctor or behavioral health professional by phone, online, or through Teladoc’s award-winning mobile app. Virtual visits are available in several languages through an interpreter, including American Sign Language (ASL).
Teladoc General Medical
Talk to a board-certified doctor 24/7 for non-emergency conditions, such as sinus pain, flu, earache, pink eye, and sore throat. You’ll get a diagnosis and prescription (if needed).
Teladoc Health Dermatology
Get convenient and reliable skincare from a licensed dermatologist for a wide range of conditions. You can use your Teladoc account to request a dermatology consult, complete a short form, and upload images of your skin issue.
Teladoc Mental Health Care
Talk to a board-certified psychiatrist, licensed psychologist, or licensed therapist from the Teladoc network by phone or video chat. Teladoc’s network of behavioral health professionals can help with concerns like anxiety, depression, grief, work pressures, and more, and you can build an ongoing relationship with a provider of your choice.
Teladoc Health (Teladoc) is a national vendor that connects individuals to board-certified physicians using HIPAA-secure video, telephone, or their award-winning mobile app. With Teladoc, our members can access unlimited non-emergency care 24/7/365.
No. Virtual care from Teladoc Health (Teladoc) is designed to handle non-emergency medical conditions and can be an alternative for a doctor’s office, urgent care center, or emergency room visit for common conditions like the flu, pink eye, or rash. However, it is not intended to replace your primary care doctor or to be used in life-threatening emergencies. You should not use Teladoc if you are experiencing a medical emergency. In case of a life-threatening emergency, dial 911 immediately.
Members can register for Teladoc Health account starting January 1, 2024 using one of the following methods:
- Call 1-800-835-2362
- Visit teladochealth.com
- Download Teladoc mobile app on Apple or Android
Once registered, you’re ready to start using virtual care from Teladoc.
With Teladoc Mental Health Care, you can talk to a board-certified psychiatrist, licensed psychologist, or licensed therapist from the Teladoc network by phone or video chat. Teladoc’s network of behavioral health professionals can help with concerns like anxiety, depression, grief, work pressures, and more, and you can build an ongoing relationship with a provider of your choice. Virtual visits are secure and confidential.
1 Diagnostic colonoscopies are subject to the cost-sharing provision of your outpatient surgery benefit.
2 Virtual care from a designated virtual provider includes telemedicine, teledermatology, and telebehavioral health services offered through our virtual care provider, Teladoc Health, an independent company.
3 Cost-sharing may apply for Catastrophic and HSA-qualified health plans.
